Resources and News
Sign up today and receive educational resources and industry updates right in your inbox!
Your Strategic Imaging Partner
As your strategic imaging partner, our mission is not limited to providing diagnostic imaging solutions, but also be a valuable resource for you and your team. We aim to keep our clients informed of industry trends and healthcare initiatives in a rapidly changing market. Contact our experts for more about how Shared Imaging’s solution can help you meet your financial, operational and clinical goals.
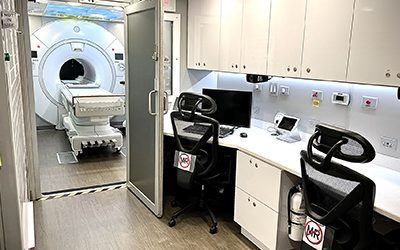
Mobile MRI in 2026: Faster. Smarter. Strategic.
Mobile MRI in 2026 has evolved from a temporary fix to a strategic solution. With rising demand, capital constraints, and AI-driven advancements, it enables faster deployment, flexible capacity, and expanded access while aligning imaging growth with financial realities.
2026 Imaging Trends
As healthcare continues to evolve at an accelerated pace, diagnostic imaging remains central to meeting clinical demand, improving outcomes, and expanding access to care. Let’s explore the top imaging trends that will shape your imaging strategy in 2026. Artificial...
Top Blogs of 2025
As the healthcare landscape continues to evolve, it becomes increasingly vital to stay ahead of the curve. In order to assist you in maintaining an efficient practice and delivering improved performance along with quality patient care, we have compiled our most...
The Smart Choice: Why a Mobile MRI Machine Makes Business and Clinical Sense
In today’s healthcare environment, leaders are challenged to deliver exceptional patient care while managing costs, space, and staffing. One solution that’s transforming how hospitals and imaging centers operate is the mobile MRI machine.Financial Efficiency Without...
Radiology Business Forty Under 40 – Amanda Forgione, CNMT
We are proud to announce that Amanda Forgione, Regional Operations Manager at Shared Imaging, has earned a place among the exceptional leaders named to the 2025 edition of Radiology Business Forty Under 40.
Cardiac PET/CT: Elevating Precision in Cardiac Imaging
In cardiovascular diagnostics, Cardiac PET/CT is setting a new standard for accuracy and efficiency. By combining Positron Emission Tomography (PET) and Computed Tomography (CT) into a single exam, providers gain both functional and anatomical insight - helping...
proven results
Shared Imaging Customer Success Stories
Maintaining Imaging Access During CT, MR, and PET/CT Replacement
See how a Northern California health system maintained uninterrupted imaging access during major equipment upgrades through a flexible, partnership-driven approach.
Mobile CT for Rural Hospitals: Maintaining Imaging Access
Learn how Shared Imaging delivered a mobile CT solution for a rural Alaska hospital, maintaining uninterrupted imaging access during construction.
Newark Beth Israel Medical Center Case Study
Capital resources and space were scarce and the required funding was simply not available to install a second MRI.
WellSpan | Ephrata Community Hospital
Shared Imaging helped minimize duplication of imaging assets and optimize service offering while meeting budgetary constraints, keeping technology up to date, and serving the patient community.
Bringing Care to the Patient
Watch to see how Kelsey-Seybold’s radiology department utilized Shared Imaging’s unique Functional Service business model to expand its diagnostic imaging capabilities to properly serve its patients.
SHARED.CARES.
Shared Imaging® believes in giving back to our local communities. Through our company initiative SHARED.CARES., we empower employees and their families to contribute time, effort, and passion towards meaningful causes within their community. Focused on health and wellness, SHARED.CARES. nurtures a company culture of giving and participating to create stronger, healthier places for our customers and employees to work and live.